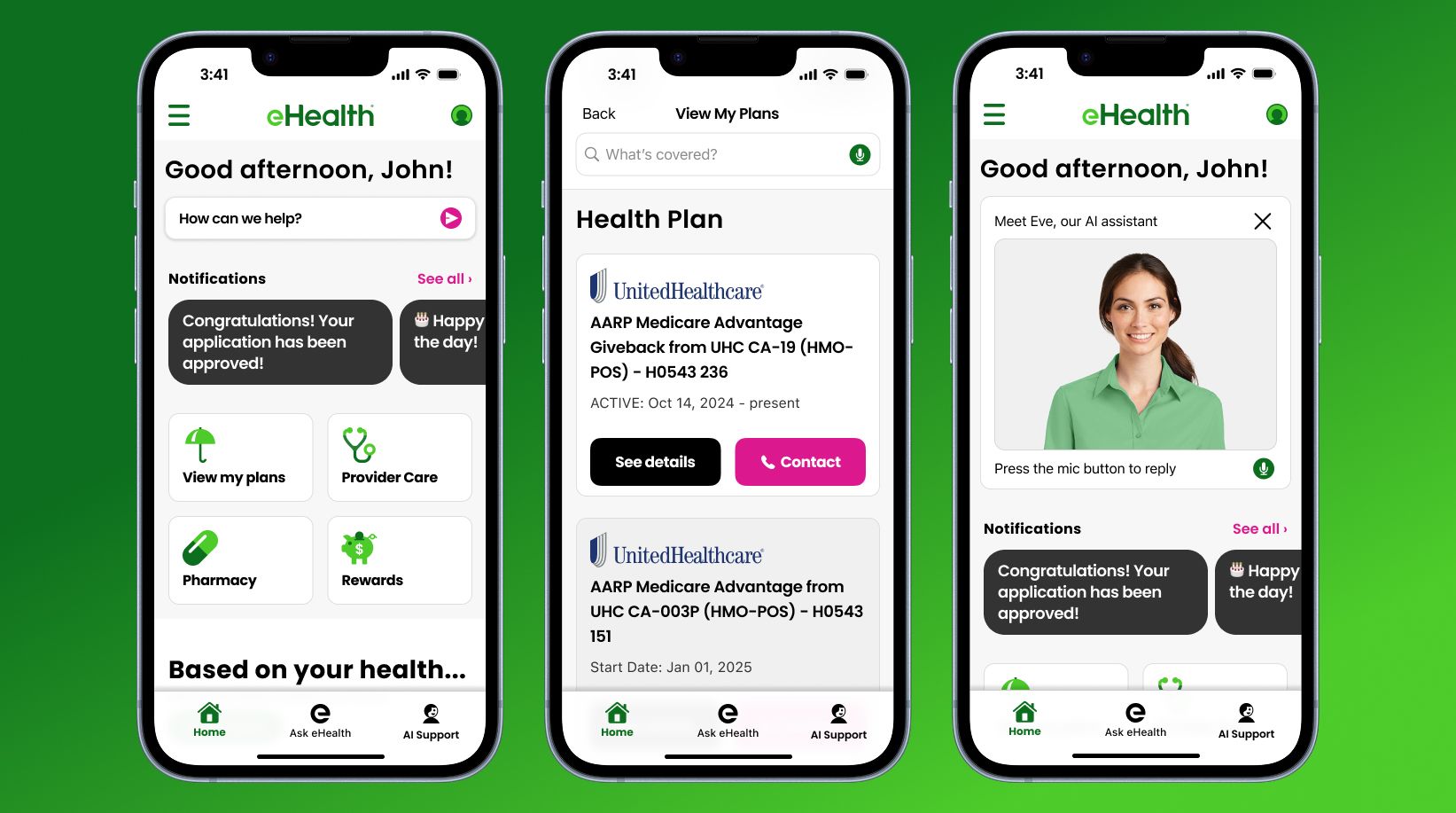
eHealth App
AI has empowered us to offer customers an app that helps them manage their health insurance, answers their questions, and continuously looks for ways to save them money or enhance their coverage.

Problem:
One of our biggest challenges of being a health insurance marketplace and broker is customer retention. After we assist a client in finding and enrolling in a health insurance plan, they work directly with their healthcare provider and carrier. Over time—often a year or two—clients’ needs evolve, but by then, they may have forgotten who helped them find their plan in the first place.
Goal:
Increase customer retention by leveraging an AI-powered virtual agent to deliver personalized health insurance plan information, respond to coverage inquiries, and generate recommendations for cost savings and optimized plan selection.
Product Discovery
We utilized a tremendous amount of existing user research and insights to inform our initial app concept and performed multiple studies as we further refined the user experience and design. We did an extensive amount of competitive research to see what features and functionality existed in carrier and provider apps in the market.
There was a clear opportunity to meet a user need that was not being met by anyone else in the industry, that being — an independent resource that provides analysis and recommendations for health insurance plans across all carriers in a specific market as a user's healthcare needs change over time.